Taking part in research — my perspective
Ron Bernstein was diagnosed with Parkinson’s in 2008. In January 2023, he decided to take part in a clinical trial, a type of research study to test a new potential treatment for Parkinson’s. Here he shares his experience.
I was diagnosed with Parkinson’s in 2008. However, I’ve been fairly lucky. Thanks to a good balance of medication, my symptoms are kept at bay.
This would not be possible if suitable drugs weren’t available. The medication I take now was developed some time ago and, no doubt, relied on people with Parkinson’s coming forward to trial the drugs. I’m very grateful to these volunteers. And so as a thank you to the past, and a contribution to the future, I decided to get involved in a clinical trial.
The study I took part in was investigating a new drug for Parkinson’s. This involved taking doses of an oral tablet multiple times throughout the day.
As this was an early stage of testing, also known as a phase 1 trial, the main aim of the study was to see how well the drug was absorbed into the body. This study was the first time that the drug had been tested in people with Parkinson’s. Although I was informed that the drug had been tested in people without Parkinson’s before I was recruited.
This comes with a degree of uncertainty. There’s a very small possibility that something unexpected could happen when a human is taking the drug for the first time. However, I was assured that every possible outcome had been planned for, and the trial was as safe as possible.
Getting ready to take part
When I registered my interest in being part of the trial, I went through a screening process that made sure that I was a good fit for the study. Then, I was invited to the research facility in London to see where I would be staying during the trial, and make sure I was comfortable, before making a final decision on whether I’d like to be involved.
The study itself involved a 17 night stay in the research facility. The facility is not exactly a hospital, but is staffed by fully qualified nurses, doctors and research staff who would be on call throughout my stay. I needed to stay in the facility so that the team could make sure I was monitored and safe throughout the trial.
When I arrived I was shown to my bed, in Bay A1 on the third floor, and made myself at home. Then I just had to wait until they called me for the first test. Every morning, I was given a schedule that let me know what to expect throughout the day. Such as when I would need to give a blood pressure reading, or a blood or urine sample.
Taking part
I thought it might be helpful to detail what tests I underwent over the 17 days. These tests were dotted throughout the day, with the earliest being 7.15am and the latest at 10pm. I hope my description of the tests makes them seem less daunting!
Blood pressure and heart rate
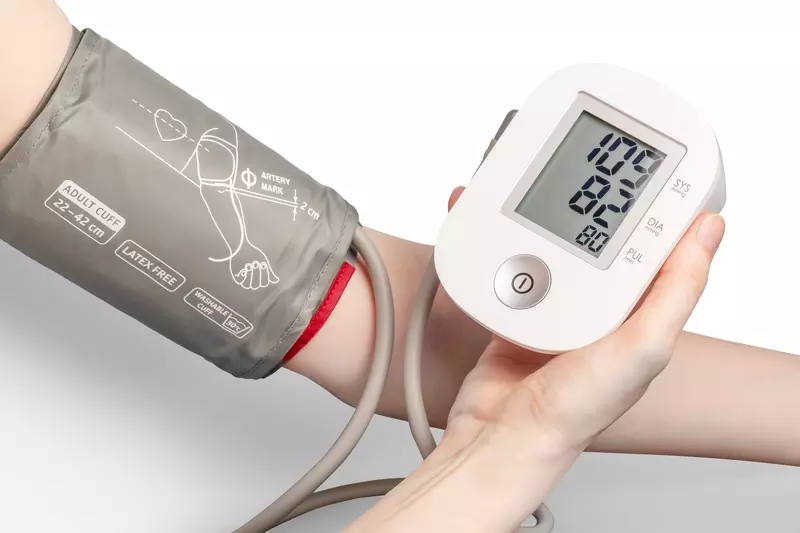
This test is non-invasive and painless. An inflatable cuff is placed around your upper arm, and then is automatically inflated until you can feel it tight against your skin. The cuff is then slowly deflated, until there is no pressure against your skin at all. Then it displays your blood pressure measurement, along with your heart rate (how many times your heart beats in 1 minute). This was the most frequent test, but only took a couple of minutes.
On three of the days, I had to wear a 24 hour blood pressure monitor so the researchers could track any changes throughout the day. This was a little inconvenient, but not too bad.
Temperature
This is another painless test. The team placed a digital thermometer just inside my ear for a few seconds to get a reading of my temperature and make sure it was stable.
Electrocardiogram (ECG)
While this test is also painless and non-invasive, it is a little more work than the first two. First, the research team placed 10 sticky patches in various places on my torso. These patches contain electrodes, which are used to capture my heartbeat and translate it to a computer, which will produce a readout. Each patch is then connected to a machine via plastic coated leads. You then just sit in the chair or bed while the machine records how your heart is working, and prints it out in real time on a piece of paper.
For me, the patches were a little uncomfortable. But I found that if I showered straight after finishing the test, and removed the sticky material, I had no trouble.

Blood samples
Please don’t be put off by this. The staff were great at making sure that they got exactly what they needed from each sample, the first time.
For each sample, a very fine needle was inserted into the vein just above my elbow. There was a sharp scratch for around a second, so I wouldn’t really call it pain. Most days I had 3 blood tests, but on some days I had to have 8 samples taken. On these days, rather than insert a new needle every time, the staff had a better solution. They applied local anaesthetic to my arm to numb the feeling in the area, and then inserted a cannula which is a more robust needle that is built to stay in your arm for long periods of time. Then they could use this to take a new sample by attaching a fresh bottle and turning a small valve, so I wasn’t bleeding the whole time!
Everyday activities
While the tests did break up the day, there was a lot of free time. I would suggest bringing along a book or a laptop for some distraction in the quiet times. I could also order a daily newspaper, or even arrange to take part in some yoga classes over Zoom!
We were allowed to have visitors too, but when I was there there was still some concern about Covid-19. So everyone had to be registered in advance, and prove they had a negative Covid-19 test before coming in.
We had 3 meals a day provided, as well as a snack before bed. I found the beds to be very comfortable and easily adjusted, and there were plenty of toilets and showers. As I was there for longer than a week, the facility offered laundry services. So I would recommend that you bring your own towel or personal comforts. No food though as that all had to be monitored and provided by the staff.
General experience
This was my first experience as part of a clinical research study, so I have nothing to compare it to. But I must say that I had a brilliant first impression. All the staff at the facility were compassionate, skilled and professional, and had the whole thing down to a fine art. They were friendly and treated me with respect, and were happy to answer any questions. I’d really like to thank all the staff involved.
Because this trial involved such a big commitment of time and many tests, I was paid for taking part in the research study. This is not always the case. But generally studies that take a large commitment will offer some kind of compensation.
There’s a lot more information you can find about taking part in research trials. But I hope this personal account has made you think about volunteering. Of course, it has a personal draw as well. Clinical studies are vital, but they take a long time. It could be up to 10 years before the drug that I’ve been involved in is available for people with Parkinson’s. I hope that we are able to benefit from it.
With many thanks to Ron Bernstein for sharing his experience with us.

